Is bone grafting common?
If you are thinking about getting dental implants, you might be told by your dentist that you need a bone graft first. Bone grafting is actually quite common. Bone grafts are often a routine prerequisite step for many dental implant patients. According to one study about half of all dental implant patients will need to undergo a bone graft procedure before proceeding with dental implant surgery. Therefore, it is reasonable to wonder what bone grafts are for, in the event you need one.
When is a bone graft necessary?
Many patients, particularly older patients, do not have enough bone in their jaws to support dental implants in the proper position. A bone graft is a way to enhance the existing, healthy bone in your mouth to accommodate and support implants.
A lack of adequate bone quantity and quality is often attributed to a process called bone resorption. However, there are many reasons why you may not have adequate bone in your mouth. These reasons may include:
- Previous tooth loss resulting in bone resorption
- Genetics
- Periodontal disease
- Injury to the mouth or jaw
- Developmental defects
It is essential to know that dental implants rely entirely on a process called osseointegration in order to stay in place. The dental implant biologically fuses with the surrounding bone tissues. As a result of successful osseointegration, dental implants provide superior stability and longterm resilience for the restoration of missing teeth.
What is a dental bone graft?
A bone graft, put simply, is the transplantation of bone tissue from one part of your body, or a donor host, to another part of your body. Bone tissue that is moved, or transplanted, will typically integrate into the surrounding tissues and provide a scaffold for the regeneration of new bone from the host. Bone grafts are used to augment the volume and quality of the bone in your mouth to provide a foundation for dental implants.
Who needs a bone graft?
If you are seeking dental implants in order to replace missing teeth, it is not uncommon to need adjunctive bone grafting to varying degrees. Those with missing teeth are susceptible to bone loss due to bone resorption and atrophy. Even those who have not been missing teeth for a long period can experience some degree of bone loss. If you have experienced partial edentulism, or complete loss of all teeth for an extended period, the chances are high that you will need a bone graft for receiving dental implants. There are also scenarios where tooth loss happens due to infections, gum disease or a traumatic injury that results in loss of bone volume in the intended area where tooth replacement with an implant is intended. A bone graft either prior or simultaneously at the time of implant placement may be required.
Why does tooth loss cause bone loss?
When teeth are lost, the underlying jaw bone surrounding the missing teeth begins to atrophy and eventually resorbs, because there are no longer teeth that require support. As a result, the body assumes that the bone that one day provided support and a means of anchorage for the teeth is no longer needed, and will gradually undergo resorption, resulting in bone deficiency. Alveolar bone is bone tissue specifically designed to hold and support your teeth. The rate and degree of alveolar bone loss and remodeling varies between individuals. Individuals with a thinner tissue makeup experience a more pronounced loss than those with a thicker biotype.
Why do I need a bone graft?
The loss of alveolar bone volume can occur before dental extraction due to periodontal disease, periapical pathology, and trauma to the teeth and bone. Additionally, the traumatic removal of teeth can cause bone loss and must be prevented. In addition, the alveolar bone suffers atrophy after tooth extraction. The resorption and remodeling of the alveolar ridge after tooth removal is a natural healing phenomenon and can negatively affect implant placement. To meet the requirements of prosthetically-guided implant placement, the remaining alveolar ridge must, therefore, be restored in most cases.
Bone grafting helps increase the volume and shape of the jaw bone available to place a dental implant. An adequate amount of healthy bone to support a dental implant is required as inadequate bone support increases the chances of implant failure and undesirable treatment outcomes.
Bone grafting is a surgical procedure that can usually be done in the dental office. It replaces the bone that has been lost with material from the patient's own body (autogenous bone) or with a natural, artificial, or synthetic substitute.
The goal is to generate new healthy and natural bone in the area of the procedure. Such grafting replaces missing bone lost from previous dental extractions, injuries, accidents, cysts, periodontal disease, infections along with many other causes. In most instances, the entire graft may be made up of synthetic or animal bone. This is commonly done where the amount of bone that needs to be augmented is small. In small-volume bone grafting, the synthetic bone occupies the space needed for the new bone to grow in and as the new bone is formed, the synthetic material gradually dissolves away.
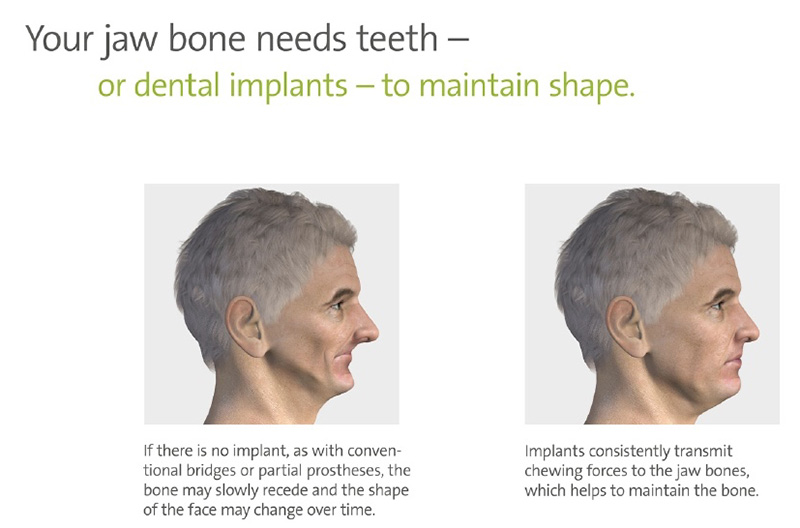
If you lose one or more permanent teeth, an indention may result in the gums and jawbone where the tooth used to be. When no longer holding a tooth in place, the jawbone recedes and the resulting indentation looks unnatural. Ridge augmentation is a procedure that can recapture the natural contour of the gums and jaw. A new tooth can then be created that is natural looking and complements your smile.
Tooth loss causes the jawbone to recede and can lead to an unnatural looking indentation in your gums and jaw, and an appearance of general aging. The original look of your mouth may not be recaptured because of spaces remaining under and between replacement teeth. They may appear too long compared to nearby teeth.
At Portland Perio Implant Center we routinely see patients that require various types of ridge augmentation for implant placement as well as pre-prosthetic correction of defects. We always use the latest techniques and materials to achieve optimal outcomes. With advances in both surgical techniques and understanding of healing processes as well as the use of regenerative biologic agents, healing times may be shorter and procedures less invasive. It is very common that a combination of procedures be performed simultaneously if indicated. These scenarios allow for placement of the dental implant and bone graft to be performed in one visit which in turn reduces the healing time, discomfort and cost of therapy.
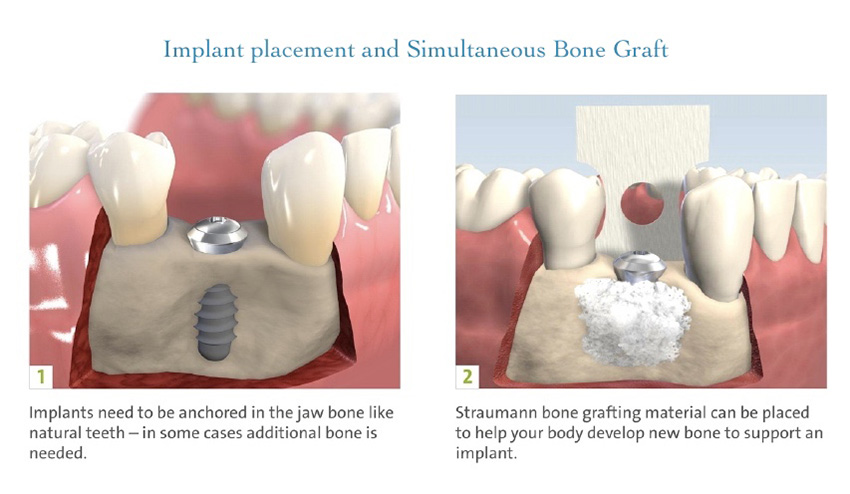
How do bone grafts work?
Dental implants are considered the gold standard treatment for replacing missing teeth. Long-term success is highly dependent on healthy peri-implant tissues (bone and gums) in adequate quantities. Thus, it makes sense that dental implants and bone grafting are often complementary procedures. Implants help preserve bone health and prevent atrophy while healthy bone volume and density provide support for implants. It is impossible to discuss one without the other. Both are essential pre-requisites for long term success, not only to restore oral health but to provide a long-lasting option for your teeth to look and function naturally.
There are several grafting techniques, depending on the site and anticipated pattern of the bone loss, the amount of bone loss, and the planned prosthetic requirements. Bone grafting is not one technique that fits all scenarios. Some of the most common methods are below:
Socket Preservation
Socket preservation is the least invasive bone grafting technique that occurs immediately after a tooth extraction, in preparation for a future dental implant. Bone graft material prepared and placed into the clean tooth socket after tooth removal. A barrier membrane is then used to cover the socket and sutured closed to protect the underlying graft. Opting for a socket graft immediately after tooth extraction can reduce the sequelae of socket remodeling and atrophy that ensues. This can help save costs down the line by avoiding the need for more invasive grafting.
The outcome of treatment with implants is no longer measured exclusively in terms of implant survival, but also by the long-term esthetic and functional success of the prosthesis. The successful esthetic and functional restoration of an implant depends on its optimal placement, which is influenced by the jaw bone dimensions. Because the ridge dimensions are so crucial, it is advantageous to preserve the dimension of the post-extraction ridge instead of reconstructing it thereafter, thus maintaining its ideal vertical and horizontal dimensions and decreasing patient morbidity.
Socket preservation is a procedure in which graft material or scaffold is placed in the socket of an extracted tooth at the time of extraction to preserve the alveolar ridge. The aim is to minimize bone shrinkage and therefore preserve the ridge width to allow a more optimal outcome for a future denture, bridge, or implant. After extraction, jaw bones may need to be preserved to keep sockets in their original shape. A significant reduction of the alveolar ridge in the horizontal dimension occurs if the socket does not receive some type of treatment.
The bone filling of the socket can be significantly improved with preservation techniques. Without socket preservation, the bone quickly resorbs. The jaw bone will never revert to its original shape once bone is lost and tissue contour has changed. Bone grafting following tooth loss can preserve the socket/ridge and minimize gum and bone collapse. There is less shrinkage and a more aesthetic tooth replacement for either an implant crown or fixed bridge around the replacement teeth.
Case study coming soon: Removal of infected tooth and socket preservation with bone graft in preparation for future implant placement.
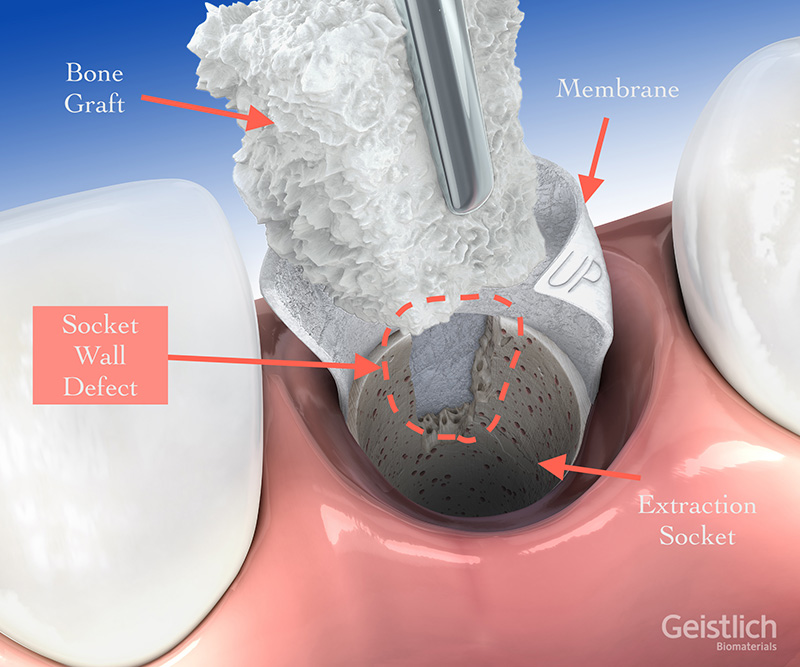
Ridge Augmentation
Ridge Grafting, also known as Ridge Augmentation, is a procedure that can recapture the natural contour of the gums and jaw. If you lose one or more permanent teeth, an indention may result in the gums and jawbone where the tooth used to be. When no longer holding a tooth in place, the jawbone recedes and the resulting indentation looks unnatural. After ridge grafting is done, a new tooth can then be created that is natural looking and complements your smile.
When socket preservation is not performed at the time of tooth extraction, ridge augmentation may be necessary at a later stage to rebuild the natural contour of the gums and jaw. This procedure begins with lifting the gum away from the jaw ridge to reveal any defects in the bone. The graft material is used to fill the ridge, or in severe bone loss cases, a block of bone is attached using screws and plates. A membrane may be placed on top of the bone graft material or block to support and secure it, and the incision is then stitched up, and the recovery process can begin.
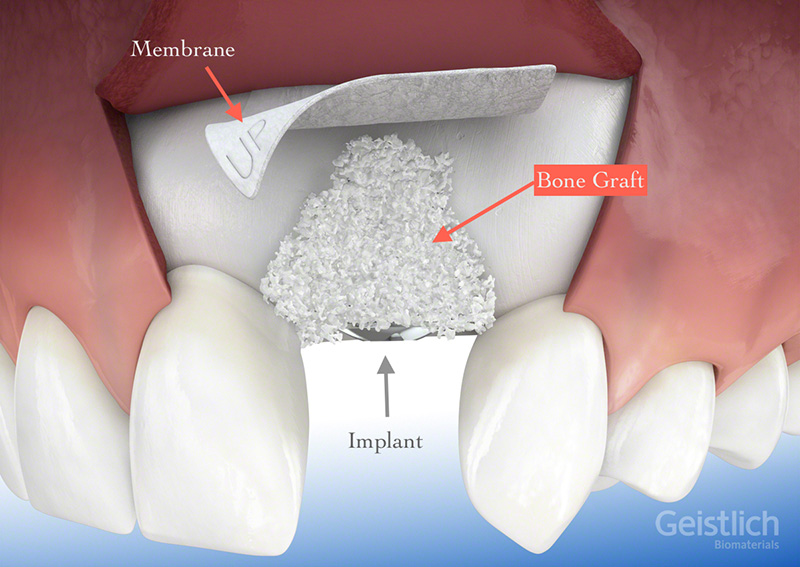
Sinus Lift
Above the roots of the molars and premolars are the maxillary sinuses that essentially are empty spaces within the bone, lined by a layer of tissue that secretes mucous. The mucous helps to humidify the air as it enters through the nose on the way to the lungs. These cells lining also contain hairlike structures that function like a broom, sweeping the mucous and any foreign particles that are trapped in the mucous, out of the sinus and into the nose where they are discharged.
When these upper teeth are removed there is both shrinkage of the socket and remodeling of the jaw bone as well as expansion of the sinus cavity into the space once occupied by the tooth (pneumatization). This natural healing process often results in a reduced vertical height of bone required for implant placement. Dental implants need bone to hold them in place so when the sinus wall is very thin, it is to place dental implants in this bone.
For implants in the back part of the upper jaw, the bone deficiency is often at the tip of the implant and bone graft is often added there via a procedure known as a sinus lift. The dental implant surgeon enters the sinus either from the side above where the upper teeth used to be (Direct Approach) or vertically through the jaw bone from below (Indirect Approach) - See Example below. The sinus membrane is then lifted upward and the donor's bone is inserted into the floor of the sinus. Remember, the floor of the sinus is the roof of the posterior upper jaw bone. After several months of healing, the bone becomes part of the patient's jaw and dental implants can be inserted and stabilized in this new sinus bone.
The timing of placement of the implant there depends on the amount and quality of bone engaged by the implant near the top of the implant instead of the tip. Implants can often be placed simultaneously at the time of the sinus lift procedure as long as an adequate amount of bone is present to engage and stabilize a portion of the implant length. The healing of the bone graft and implant integration takes place together. If not, then it is prudent to wait a few months before the insertion of the implant.
The sinus graft makes it possible for many patients to have dental implants when years ago there was no other option other than wearing loose dentures.
Prior to sinus grafting a 3D image of the sinuses is obtained to exclude the presence of pathology and visualize the space in greater detail for diagnostic and planning purposes.
Bone Ring
Portland Perio Implant Center was the first center in Oregon to complete the necessary certification training and subsequently implement the Allograft Bone Ring grafting technique when it was introduced to the US market in 2017.
The technique and materials have been available in Europe, where it was developed, for many years. Conceptually the Allograft technique is similar to those previously reported with the autogenous bone cylinder but has the major advantage of reduced morbidity to the patient since a second surgical procedure is not necessary.
Although this method aims to simplify, shorten treatment length and make implant placement possible in areas that generally require staged bone grafting with a minimum of 6 months healing period, it is a technically advanced technique that requires surgical expertise in the field of bone augmentation and implant therapy.
Implant restoration in the edentulous jaw often requires additional augmentation measures on account of the physiological remodeling and resorption processes following tooth loss and the associated reduction in bone availability. This grafting technique has been successfully used for bone augmentation in sinus lift procedures, significant ridge defects as well as challenging vertical ridge grafting in the posterior arches.
This method eliminates many of the problems associated with autogenous grafting. Since bone used for autologous grafts is usually obtained from intraoral donor regions, little autologous bone is available for augmentation. Other disadvantages are that the additional intraoral bone harvesting procedure is stressful for the patient and can increase the risk of potential postoperative complications at the donor site, including pain, infection, and altered sensation.
Unlike the current method of harvesting intraoral bone in block form, the bone ring is a simple possibility of obtaining Allograft donor bone in ring form and performing reconstruction of three-dimensional defects. This procedure enables a one-stage minimally invasive procedure for a bone graft to be combined with simultaneous implant insertion in significant defects. This translates to less patient stress and greater patient acceptance. Utilizing the bone ring method, primarily stable implant insertion is achievable in a one-stage procedure even when local bone availability is low.
Case Study
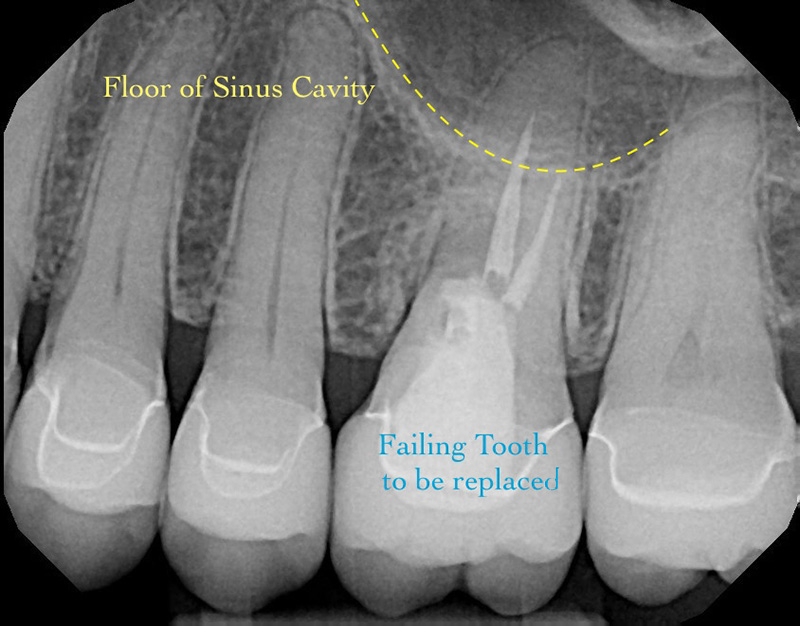
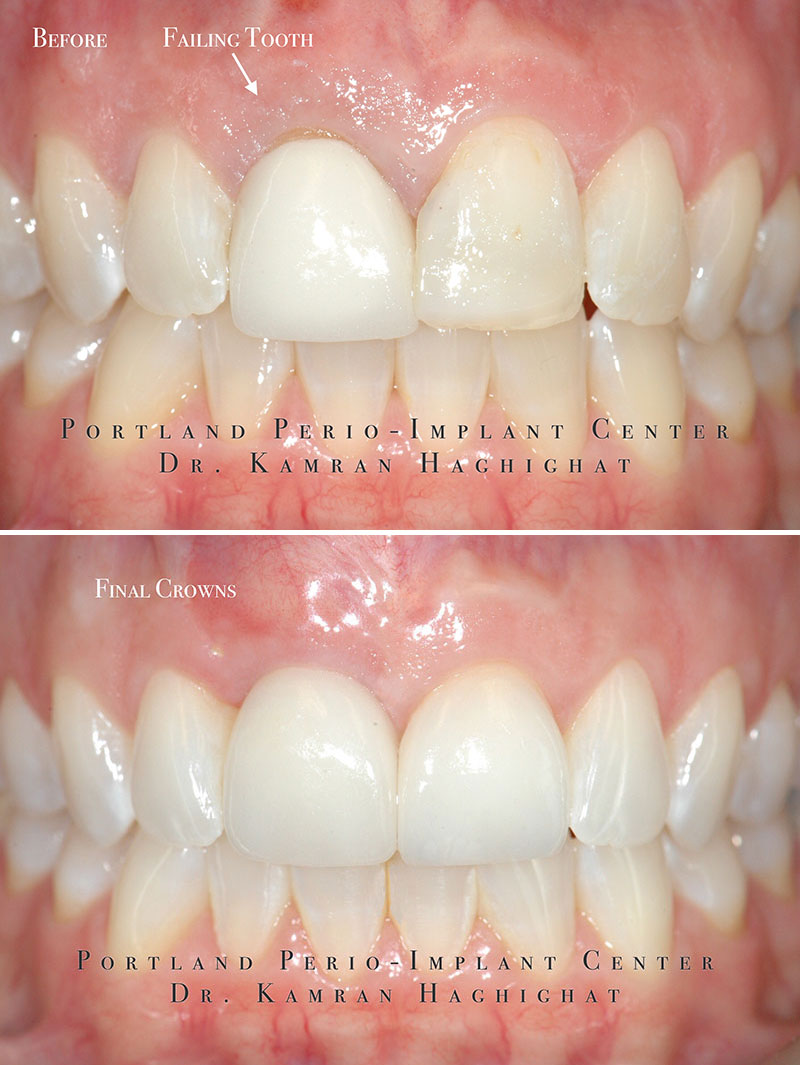
Our patient Lori was referred to the Portland Perio Implant Center for evaluation of a front tooth that was previously traumatized and required removal. Her chief complaint was the esthetics of the front upper right central incisor tooth (#8) that was slightly extruded and had become progressively more mobile. A thorough clinical and radiographic assessment, including a CT scan, revealed extensive bone loss along the facial aspect of the tooth.
In conventional implant therapy, placement of an immediate implant following tooth extraction would not be advisable in such scenarios. Such cases typically follow the staged treatment protocol where bone grafting is performed first, followed by implant placement after a six-month healing phase. Therefore, it becomes an inconvenient and undesirable proposition for patients that need to prepare for therapy that may take as long as one year to complete. With the Allograft Bone Ring technique, treatment times are typically reduced by as much as 4 to 6 months as the implant and bone graft are done simultaneously.
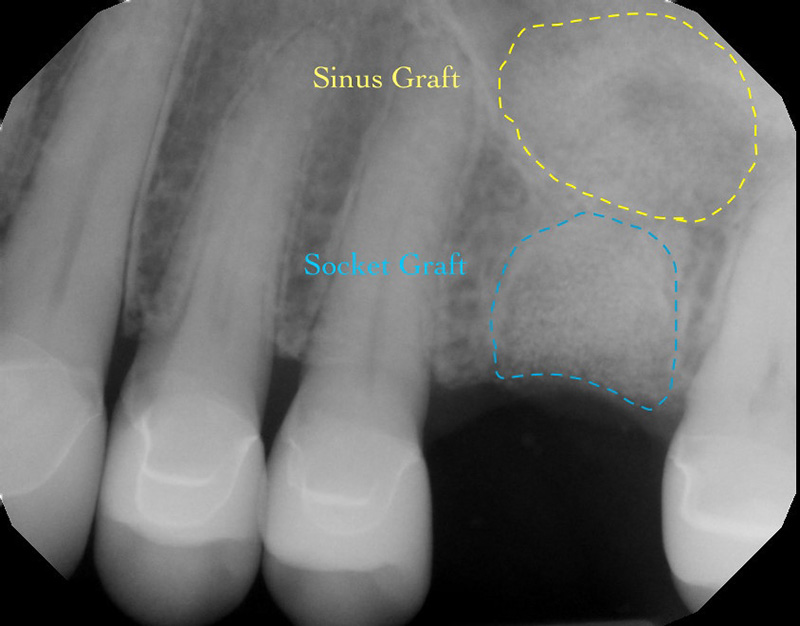
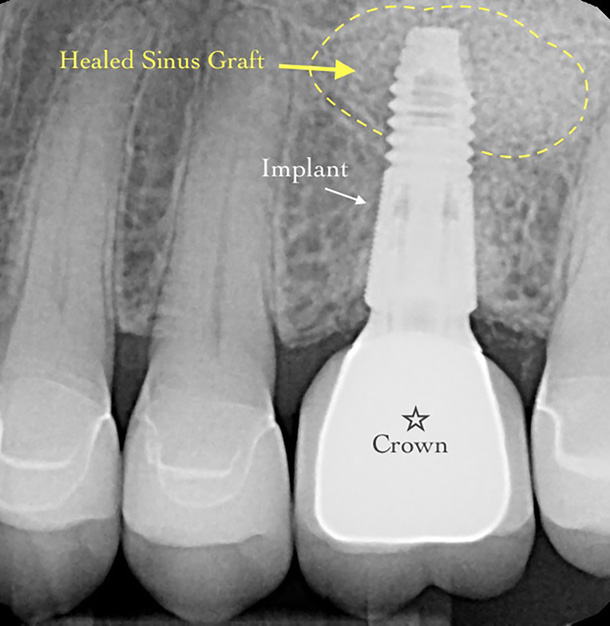
Lori was relieved to hear that our experience with the Allograft Bone Ring method would shorten her treatment time. We were able to remove the failing tooth, immediately place a dental implant, and graft the area.
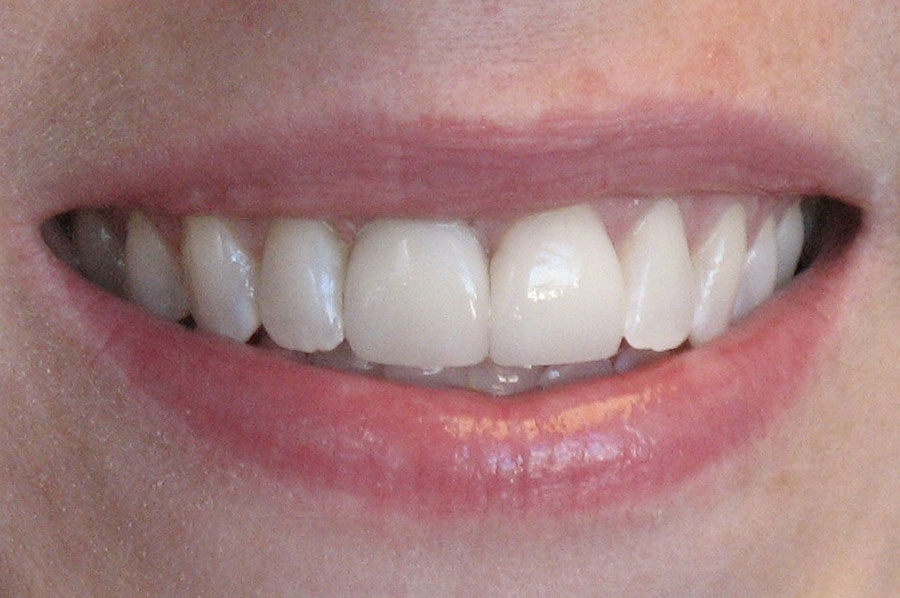
What material is used for bone grafting?
Bone grafting is a surgical procedure using transplanted bone to regenerate and repair damaged bone, so the restored jawbone becomes a strong foundation for an implant. During implant placement surgery, a small titanium post, which acts as the “root” of a tooth, is placed under the gums and secured deep into the jawbone. Much like inserting a nail into wood, the wood needs to be dense enough and wide enough for the nail to anchor itself. Similarly, a bone grafting procedure increases the volume and density of the jaw bone, so the implant post is secure.
There are several types of bone graft materials to rebuild a jawbone:
Synthetic bone material
Also known as alloplasts. These are synthetic materials developed in a lab to replace human bone. Synthetic bone is the most affordable material on the market and readily available.
Your own bone
Also known as autografts, you can extract your own bone tissue for use as grafting material. Bone can be taken from the back of the jaw, chin, hips, or legs. Opting to use your own bone material does come with drawbacks. For one, choosing an autograft may require hospitalization which will entail additional hospitalization costs. There may be additional healing time as well, with two surgical sites.
Other human donor bone
Also known as allografts, you can also receive grafting material from a donor body. The cadaver bone material is sterilized to eliminate any bacteria or other biological materials. Donor material is not as commonly used as synthetic material or materials from your own body.
Bone from animals
Also known as xenografts. Bones from animal sources such as cows similarly undergo treatments to render it safe and sterile for use.
After deciding which bone graft material is most suitable, the goal is to use the bone tissue to graft onto the jawbone. The cells inside the bone graft material provide a framework to spur the growth of new, healthier bone tissues in the jaw.
Is a bone graft painful?
While a “bone graft” may sound painful, in reality, the procedure itself is painless with the use of anesthesia. The vast majority of bone graft patients report no pain whatsoever during the operation. Aside from the prick of the needle delivering anesthetics, you will not need to worry about feeling pain while the doctor is placing the graft. Local anesthesia completely numbs the site of the graft.
After the procedure is complete and the anesthesia wears off, most patients still report little to no pain even during the recovery period. While you may experience minor discomfort, for the most part, the recovery period should be relatively comfortable. Minor postoperative pain can be alleviated with readily available painkillers and should go away after a few days.
If your oral pain does not disappear or lessen over time, it could be a sign that your graft has become infected. However, this should not be a concern with proper aftercare.
Does everyone need a bone graft before getting dental implants?
Not every patient needs a bone graft before dental implants. It is impossible to tell whether or not you require graft without an in-person consultation and oral checkup. However, as a general rule of thumb, patients under the age of 50 with no prior signs or symptoms of periodontal disease and no history of missing teeth will likely be okay without a bone graft. Older patients, those with periodontal disease, or those with missing teeth, will probably need a bone graft before getting implants as a result of jawbone loss.
Teeth are anchored in place to the jawbone. Similar to a muscle, bone tissues need to be stimulated or “exercised” through motions such as chewing and biting to maintain its shape and volume. As soon as a tooth is extracted or lost, the jawbone is no longer stimulated, and atrophy takes hold. This is known as bone resorption. Resorption is when the body thinks the bone is no longer needed, and thus, the bone starts to break down. Within the first year of tooth loss, up to 25 percent of the bone may deteriorate.
Other reasons for jawbone loss, besides lost or extracted teeth, include periodontal (gum) disease, injury or trauma, ill-fitting dentures, and infections. Due to bone loss, there may not be adequate width, height, or density of bone at the site for successful implant surgery. If this is the case, a bone grafting procedure is necessary.
There are many reasons for a bone graft prior to receiving dental implants. The following are the top four benefits of bone grafting and why it complements dental implant surgeries:
1. Rebuilds the thickness and density of the jawbone
It’s a necessary step for successful dental implant surgery. It rebuilds the thickness and density of the jawbone to provide a strong foundation to support a long-lasting implant.
2. Avoid future costs
It saves additional costs and complications down the line as an implant could fail over time if there is not enough bone. Even if dental implants are not considered at the time of tooth loss, socket preservation should be considered so that dental implant surgery can be a viable option in the future.
3. Complements implant surgery by restoring function
It is widely accepted that dental implants restore oral health, but it’s only part of the equation. A shrinking jawbone can impact everyday tasks such as speaking, eating, and other routine activities.
4. It maintains the shape of the jawline
Another means to help you look and feel like yourself. The allure of dental implants is that they look, feel, and function like natural teeth. It makes sense to also restore the natural contours of your jaw and gums to looking, feeling, and functioning naturally as well. Without bone grafting, your implant may look natural for a time, but the shape of your face and jawline can change over time as the jawbone recedes.
Undergoing a bone grafting procedure before receiving dental implants is quite common. However, they are not always required for successful dental implants, and may not be right for everyone. Portland Perio Implant Center will evaluate and determine whether bone grafting is necessary on a case-by-case basis.
What happens after the bone grafting procedure?
After your bone graft surgery is finished, make sure to take the medications prescribed by your periodontist. This will help keep your wound in good shape and prevent infections. Practice basic oral hygiene as well and there should be little risk of a bacterial infection. You will receive more detailed instructions after your surgery.
In general, the majority of patients who receive a bone graft experience minimal discomfort that is alleviated by analgesics. Pain perception however, varies from one individual to another based on one's tolerance As long as antibiotics as prescribed, very few patients suffer any setbacks during the recovery period.
Patients who experience pain after a bone graft procedure can usually take basic pain medications containing ibuprofen or acetaminophen unless contraindicated. If you experience worsening pain, especially pain that is accompanied by swelling and fever, you should contact us immediately. Severe pain is not a normal part of the post-bone graft recovery process.
The recovery period is mostly a waiting game. Your graft needs time to integrate and fuse with surrounding natural bone tissues. Unfortunately, there is no exact timeframe for this process to occur. Bone graft healing times range 4-8 months based on nature and extent of the procedure.
To keep an eye on the progress of your bone graft, your surgeon will have you come for regular checkups. Once it is determined that your graft is completely healed, then you can proceed with your dental implant placement.
Some helpful “next steps” after a bone graft procedure include:
Consultation
Debrief with your periodontist or dentist about your overall procedure experience, questions, and concerns going forward.
Pain
Take over-the-counter pain medications, such as Advil or Tylenol, to relieve any potential postoperative pain.
Avoidance
Avoid touching your graft with your tongue as much as possible.
Eating
Eat soft foods for a few days after your procedure.
Activity
Avoid physical activity for a week following your bone grafting procedure.
Healing
Be patient. The healing process can take some time.





