The Complete Guide To
Zirconia vs. Titanium Dental Implants
Contents
Types of Dental Implant Materials
Zirconia vs. Titanium: Pros & Cons
Advantages of Metal Free Zirconia Dental Implants
When To Choose Titanium vs. Zirconia Dental Implants
CHAPTER 1
Introduction
Titanium dental implants demonstrate excellent biocompatibility and offer numerous treatment possibilities to improve patients’ quality of life. Nevertheless, questions regarding sensitivity to titanium have been arising in recent years. It has been claimed that some patients could develop clinical signs of hypersensitivity to titanium, and the inadequacy of conventional epicutaneous patch tests in detecting such allergies has been established. The MELISA® test is perhaps the most accurate available and the prevalence of titanium allergy has been estimated at 0.6% using this method. As a result the notion of an alternative to titanium implants has been growing for almost 40 years.
Zirconium dioxide (zirconia) ceramics with improved properties have been introduced as an alternative material to aluminum oxide. They were first used for the fabrication of crowns and implant abutments. The white opaque color of zirconia, along with early reports of good biocompatibility and low affinity to bacterial plaque, making it a material of interest in biomedical sciences. Zirconia also exhibits several promising physical and mechanical properties, including low thermal conductivity, high flexural strength, as well as wear and corrosion resistance. However, one of zirconia's negative properties is its low-temperature degradation or aging. In the presence of water or water vapor, progressive deterioration of the material is seen.
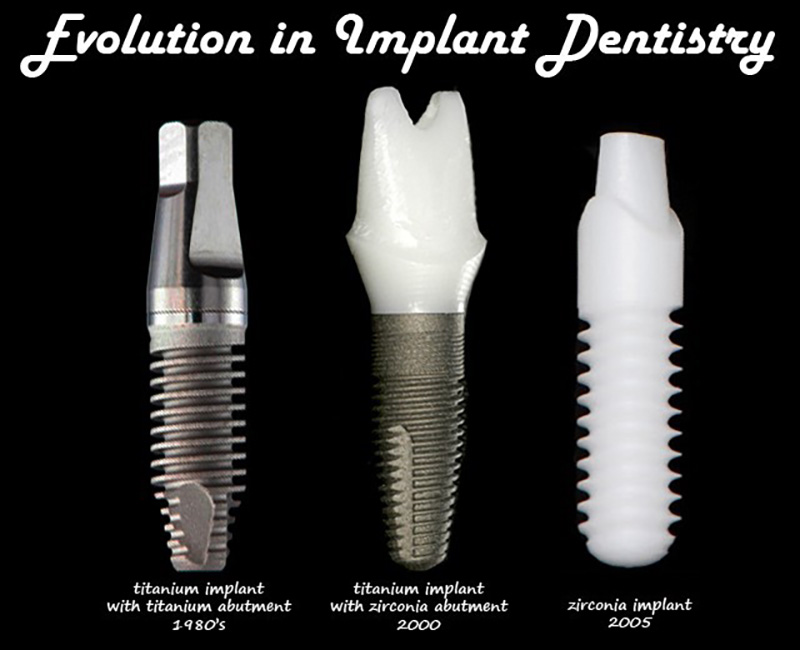
At present, only a few ceramic systems offer two-piece implants. Currently, the majority of zirconia implants produced are one-piece implants. However, such systems have several limitations. The surgical placement of the implant may not always meet the prosthodontic requirements, and angled abutments to correct misalignment are unavailable. Secondary corrections of the shape by grinding much be avoided as this severely affects the fracture strength of zirconia. Cementation is the only option for connection prosthodontic elements to one-piece implants. An increased risk for inadvertently leaving excess luting cement in the submucosal area may induce local infection, which occasionally instigates substantial tissue damage.
The major technical complication appears to be a fracture of the implant. Osseointegration (or bone-implant integration) is a major factor in the success of modern dental implants. Titanium remains the material of choice for obtaining and maintaining this phenomenon.
From a biological point of view, zirconia presents with interesting assets. It has demonstrated a low affinity to bacterial plaque, small amounts of inflammatory infiltrate, and has good soft-tissue integration. These properties might lower the risk of peri-implant diseases.
Early failure rates of zirconia implant systems developed and tested so far were generally higher compared with titanium implants. Solid data on long-term outcomes is scarce. Technical failure as a result of fracture of the material is a sensitive issue and a critical factor for usability and acceptance in daily practice.
There is room for further technical progress of currently available zirconia implant systems. More clinical investigations need to be carried out to identify all relevant technical and biological factors with an impact on the success and patient satisfaction. At present, the evidence for a final verdict is still incomplete and the field is still changing in many ways.
As there is more awareness of the availability of zirconia implants on the market, we are available to discuss this option with you and see if it's a suitable option for your situation.
CHAPTER 2
What Are Zirconia Dental Implants?
Zirconia vs. Titanium Dental Implants: Which Is Best For You?
Zirconia and titanium are by far the two most readily available and widely used materials for dental implants today. Both are high quality, inert, dental grade, and safe materials that allow for natural osseointegration between the implant and underlying bone to occur. However, many patients wonder which implant material is best for them.
Let’s find out more.
Titanium implants are either grade 4 commercially pure titanium or grade 5 alloy containing titanium (6AL-4V). Grade 5 titanium alloy implants are harder than grade 4. Both have over 85% titanium composition, which produces an oxide layer over the implant to aid in bone integration. These are the most commonly used and researched dental implants and have a long-term success rate of 94-98%.
What Are Zirconia Dental Implants?
Zirconia dental implants are dental implants made from zirconium oxide. Zirconia is considered a no-metal, white ceramic material due to its crystalline structure. Zirconia is in fact, a transitional metal, but in its oxide form is referred to as a ceramic material. Many dental clinics consider zirconia to be a porcelain alternative in a variety of cosmetic dentistry applications such as dental crowns, and has gained popularity in holistic-based clinical models. Zirconia as a dental material was introduced to the general public in the late 1980s.
In the case of dental implants, zirconia provides superior compressive strength and sufficient lateral strength for most dental implant scenarios. Furthermore, zirconia is naturally white, which is visually more appealing to many consumers.
It is important to note, however, that the visual results produced by titanium implants can be made to be aesthetically identical to those of zirconia implants. However, in some patients with thin bone or gum tissues, the gray titanium implant may be visible. In this case, a zirconia implant should be used to avoid the appearance of a gray line or visible gray coloration.
Nonetheless, many still opt to pay extra for zirconia for a variety of perceived benefits. Zirconia is, for example, allergy-free. Furthermore, some patients have reservations about placing outright metals in their mouths and subscribe to notions of holistic dentistry. These patients may be concerned about galvanic toxicity which has been associated with metal-based applications. It is important to note, however, that true allergy to titanium is extremely rare, with less than 0.6% prevalence report in the literature.
Early zirconia implants were often designed as “single-piece,” monolithic dental implants. What this means is that there was no separate abutment piece. This created limitations in its application, such as in cases that required submerging the implant during the healing period. The new generation of zirconia implants are produced in the traditional two-piece configuration, which provides for more versatility.
Characteristics of Zirconia Implants
Highly durable
Ceramic qualities
White coloration
Superior aesthetics
Transitional metal
Extreme compressive resistance
Less ductile than metal implants
Chemically inert
Acid-resistant
Monolithic one and two piece implant designs available
Non-allergenic
Osseointegration-friendly
Premium price
CHAPTER 3
What Are Titanium Dental Implants?
Titanium dental implants are the go-to choice for many implant specialists in the field today. Titanium has been used as an implant material since the 1960s and has a long and successful history of producing excellent results in oral applications, with long term success rates that range from 94% to 98%. Titanium implants are either made from grade 4 commercial pure titanium or grade 5 alloy containing titanium (6AL-4V). Grade 5 titanium alloy implants are harder than grade 4, with both having over 85% titanium composition. This produces an oxide layer over the implant that aids in bone integration. These are the most commonly used and researched dental implants.
Titanium implants can last for 20 years or longer with proper care and oral hygiene, with survival rates of 30+ years documented. Clinics that specialize in dental implant therapy can report success rates over 97%. The risk of an allergic reaction to dental-grade titanium implants is incredibly minuscule. A massive clinical study of 1500 consecutive patients found an allergic reaction prevalence rate of only 0.6%. What this means is that the vast majority of patients should not be concerned about developing an allergic reaction to commercially pure dental-grade titanium materials.
Titanium implants typically consist of three components: the metal post which is embedded in the jaw and hidden from view, a separate abutment piece which acts as a support for a prosthetic attachment, and the final crown which is the visible portion of a replacement tooth.
Characteristics of Titanium Implants
Highly durable
Metal material
Extreme compressive resistance
Excellent resistance to lateral forces
Rare allergy risks
Chemically inert
Acid-resistant
Osseointegration-friendly
Widely used with 40+ years of data
CHAPTER 4
Zirconia vs. Titanium: Which Are Best for Dental Implants?
Both zirconia and titanium are excellent materials for use in the fabrication of high-quality dental implants. However, whether to use one type of implant material over another depends entirely on the case and individual patient at hand. There is no easy answer. Instead, it is essential to take all the particular facts of each patient’s situation into account, including their personal needs and desires. Patients who prefer a solution that adheres to notions of “holistic dentistry” would opt for zirconia implants, even if titanium will serve just as well. Likewise, patients who are allergic to dental-grade titanium (extremely rare) and confirmed by sensitivity tests like MELISA (despite false-negative results) will likely want to choose zirconia over titanium.
Outside of personal preference or limiting factors, there are many other occasions where one solution may be preferable over the other. Here are just a few general considerations many patients take into account when choosing between zirconia and titanium implants.
Consult A Dental Implant Specialist To Know
As you can see, both zirconia and titanium implants are viable solutions with similar success rates. However, which implant material to choose in a particular case can’t be definitively answered without taking into account your individual needs. To determine which type of implant to choose, assess your own goals for the dental implant process. Figure out your must-have implant characteristics, and schedule an appointment with a dental implant specialist. Consulting with an experienced and knowledgeable implant expert will go a long way towards determining whether zirconia or titanium is best for you.


